Methadone
Overview
Popular names ‘juice’, ‘meth’, ‘green’
What is it?
Methadone is a man-made (synthetic) form of heroin. It is a strong painkiller often used in the treatment of heroin addiction.
Sought after effects
- long-lasting and smooth action
- prevents heroin withdrawal symptoms
Undesired effects
- none of the pleasurable effects attributed to recreational opiate use
It is an addictive drug in its own right, producing tolerance and its own withdrawal syndrome.
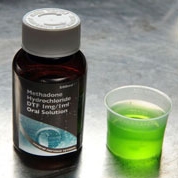
What does it look like?
It is available on the street, and usually comes in the form of a sticky green liquid; the liquid mixture is made in other colours however, and also in tablet form.
How is it taken?
Swallowed: both the liquid and tablet forms are made for swallowing (ingesting)
Injected: ampoules for injection are produced but are prescribed to relatively few heroin users.
